There are trillions of microorganisms everywhere throughout your body. It’s estimated that there are millions of bacteria in each square centimeter of skin.
An estimated 300-500 different bacterial species can be identified in your gastrointestinal tract.
Only a small number are dangerous and cause problems (pathogenic). The vast majority of these microbes are harmless (opportunistic), and many are even critical for promoting good health (beneficial).
Your Skin’s Microbiome
The micro-ecosystem on your skin can fluctuate by daily influences such as humidity, temperature, pH, lipid levels, diet, exercise, medications, and stress.
Some bacteria thrive in moist microenvironments (Staphylococcus and Corynebacterium, for example), while others favor a more oil setting (Propionibacterium).
An essential role of the skin microbiome is maintaining the skin’s barrier function, which helps keep moisture in and environmental irritants out. It also helps to regulate the immune system and inflammation.
The various organisms can compete for space and resources, and when too many pathogenic bacteria thrive, this can lead to health issues.
When the microbiome is a healthy ecosystem, the beneficial bacteria prevent the pathogenic bacteria from taking over, protecting you from harmful infections.
Probiotics, Prebiotics, Postbiotics, Antibiotics
Probiotics are defined as “live microorganisms which when administered in adequate amounts confer a health benefit on the host.”
Another term you might hear is prebiotics, food for beneficial bacteria. They are ingredients that stimulate the growth and activity of beneficial bacteria.
Postbiotics are the metabolites or byproducts of bacteria for beneficial effects without administering live microorganisms.
Antibiotics kill or inhibit the growth of bacteria, often indiscriminately. These medications can effectively eliminate pathogenic bacteria and wipe out the beneficial bacteria and cause other side effects. Combination therapy uses antibiotics and probiotics to restore a healthy and diverse bacterial population.
Probiotic Therapy For Your Skin
Probiotics have been shown to decrease the incidence of infections and the need for antibiotic therapy while improving wound healing and markers of inflammation.
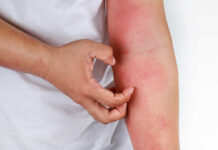
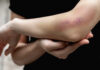
Probiotic bacteriotherapy appears to be a safe and effective strategy for preventing and treating skin diseases like atopic dermatitis and acne and might be helpful for rosacea, psoriasis, and eczema, though more studies are required.
Atopic dermatitis is associated with a high concentration of pathogenic Staphylococcus aureus, leading to immune dysfunction and disruption of the skin barrier. Introducing more beneficial bacteria into the microbiome with probiotics may help to reduce the number of pathogenic bacteria and improve the symptoms of atopic dermatitis.
Topical probiotics reduce acne lesion concentration by improving the skin barrier and controlling the overgrowth of pathogenic bacteria associated with acne.
Probiotics may also help improve skin hydration and decrease skin over-sensitivity through barrier-strengthening effects.
While more research is needed, the evidence gathered so far suggests probiotic therapy can be a promising treatment for various skin conditions.
If you’re interested in trying probiotic therapy for your skin, speak to your health care provider about the best way to proceed. Not all probiotics or interventions work for everyone, and the most effective strategy might involve a combination of topical and oral probiotic and antibiotic medicines.